Cancer is a deadly disease that does not discriminate. Anyone of any age, any gender, and any ethnicity can be diagnosed with cancer. But although many cancers are preventable or manageable with routine care and screenings, Latinos have higher rates of preventable, infection-related cancers, according to a study from the American Cancer Society.
The report shows that, while Latinos have lower cancer incidences overall than non-Hispanic whites, they have much higher rates of certain preventable cancers. This is often attributed to less access to care and less education around screening options and disease warning signs.
The disparities around healthcare, cancer screenings, treatments, and education are undeniable, and Latinos and other minority populations are paying the price.
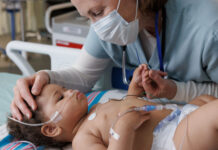
Just ask Yla Flores, a Latina cancer survivor diagnosed with stage III colorectal cancer after an at-home screening, followed by a colonoscopy that confirmed her diagnosis.
Flores’s journey included removing over a foot of her colon and six months of chemotherapy following her cancer diagnosis. While she is a survivor, the fate of other minority cancer patients is not always such a happy ending.
Her cancer was diagnosed at a later stage, as it is so often with minority patients, making the disease more challenging to treat and may lead to a more devastating prognosis. Flores is now on a mission to share her story and inspire and educate others on the importance of cancer screenings to prevent and/or find cancer early.
“Before my diagnosis, I never thought I might be at risk for colon cancer. I had zero symptoms. That’s what makes this so scary. The assumption is that you should have some type of symptoms to give you a clue that something is wrong,” Flores told BeLatina.
Research confirms a disparity in the Latino community where cancer screenings and treatments are concerned, and Latino individuals are vulnerable to healthcare inequalities, particularly with cancer and other deadly (but sometimes preventable) diseases.
“Being a first-generation American myself, I saw my parents work really hard and hardly ever miss a workday. They would never see a doctor unless they were sick,” said Flores. So, the fact that minority communities are often diagnosed later in their cancer journey was a harsh reality she knew all too well.
Thankfully, she took an at-home screening test that saved her life. But many individuals in minority communities are not quite so lucky.
How Cancer Impacts Minority Communities
The study, published in CA: A Cancer Journal for Clinicians, a flagship journal of the American Cancer Society, found that while Hispanics have 25 percent to 30 percent lower overall cancer incidence and mortality rate than non-Hispanic whites, they have higher rates of cancers which are attributed to less access to care and screenings. The study also estimated that there will be 176,000 new cancer cases and 46,000 cancer deaths will occur among Latinos in the continental U.S. and Hawaii this year.
In terms of which cancer types are most prevalent and deadly in the Latino community, the study found the most common causes of cancer deaths among Latino men are lung, colorectal, and liver cancers. Among Latinas, the most common are breast, lung, and colorectal cancers.
Cancer is less prevalent overall but is often misdiagnosed or diagnosed later and therefore tends to be more difficult to treat, indicating a major disparity in the Latino population. Experts agree that Latino communities are often living below the poverty line, with a high percentage of individuals uninsured, which leads to a lack of prompt diagnosis, lack of screening, lack of preventative healthcare, and lack of access to treatment.
“One thing that research has shown is that Hispanic and Latinx individuals are more likely to live below the federal poverty level, attain lower education levels, and live in disadvantaged neighborhoods compared to white individuals,” explains Dr. Lindsey S. Treviño, Ph.D. “This also goes for other minority communities and backgrounds such as African Americans,” Dr. Treviño explained to BeLatina. “And for individuals who fall under these categories, keeping up with the basic needs of day-to-day life is all they can focus on.” This means that preventative care is often considered a luxury that they just cannot afford and cannot focus on.
In addition, individuals in minority communities are often unaware or uneducated on the risk factors to consider when thinking about cancer and other diseases.
They might not know of family history or of other relatives who have been diagnosed with cancer. They might not be aware of other risk factors such as genetic predisposition, obesity, diabetes, and dietary risks. They might not know what symptoms to look for, and they might not even have a true baseline for health if they cannot access routine healthcare when they are healthy, before any diagnosis.
Treviño is an Assistant Professor, Division of Health Equities, Department of Population Sciences at the City of Hope, an NCI-designated Comprehensive Cancer Center. She believes strongly that creating a shift in how Latino communities understand and approach preventative healthcare, especially where cancer is concerned, requires that experts, researchers, and medical practitioners work together to communicate with culturally appropriate information.
“In the healthcare field, especially the cancer field, we’re currently trying to address the lower use of prevention screening among minority populations,” said Dr. Treviño. But it’s not as simple as just offering up information. Practitioners and experts must be careful how that information is communicated. “It all goes back to trying to message properly and ensure that the message goes out to the right people so that we can address this disparity,” she explained. “When you think about prevention screening and prevention tools, the language used really needs to be culturally appropriate and accessible. We need to think about our audience. We need to ensure that the messaging is in a language these individuals will understand. Is it culturally appropriate? Is it sensitive to their cultural beliefs about health and family?”
Financial burdens are associated with healthcare and cancer treatments, which often prevent minority communities from accessing screening and seeking medical assistance with illness. “The issue of insurance is a big one. Because research has shown that Hispanic and Latino individuals often receive a lower quality of care in comparison to white individuals, and quality care includes receiving guideline-recommended care, which should be standard,” explains Dr. Treviño.
This is not a trivial issue because the quality of care, and access to quality cancer care, is often directly linked to health insurance status, and “we know that Hispanic and Latinx individuals are more likely to be uninsured or underinsured,” she continues.
Thankfully, organizations are on a mission to ease these burdens by spreading information and offering guidance to the Latinx community. For example, Latinas Contra Cancer is a non-profit organization that helps people navigate the insurance world where cancer treatment and healthcare are concerned.
Another factor to consider is the stigma around healthcare and cancer screenings.
Many individuals in minority populations worry about discrimination and racism should they need screening or treatment. They also might not even be aware or educated on the types of screenings and treatments available to them. If that information is not appropriately communicated so that the Latino community will understand, it leads to a lack of action and misdiagnoses.
If you or a loved one is dealing with a cancer diagnosis or needs guidance and information, there are many useful tools online that can help. “The American Cancer Society has a great resource for people who might have questions, including information on screening, prevention, and treatment options. This is one of the best resources, published in English and Spanish for people who need guidance,” said Dr. Treviño.
Clearly, while cancer is a deadly disease that can and does impact everyone and anyone, it doesn’t affect everyone equally, which is a real problem for many Latinos today.
Taking Steps to Protect the Latinx Community One Screening at a Time
Yla Flores is an example of resilience, survival, and a happy ending when a cancer diagnosis was not the end but the beginning. Flores’s at-home screening literally saved her life, a reality she does not take for granted, and it all started with a routine exam and a discussion about her health in a way that was accessible. “I went to a well-woman exam, and my doctor recommended Cologuard®. She recommended this screening method so I wouldn’t have to miss time from work,” she said. “At the time, I did not feel I was educated on different screening options. When my doctor told me about Cologuard®, I was relieved not to have to be put under for a colonoscopy.”
Flores’s story exemplifies why education and awareness are so crucial in minority communities. Many people are not aware that at-home screenings are even an option, let alone that they could provide life-saving results.
Thankfully, efforts are being made in the medical and research communities to address these access issues and these healthcare policies. “But we still have a long way to go,” admits Dr. Treviño. “I’m a firm believer that it’s going to take effort from patients, their caregivers, their family members, plus healthcare providers, plus the researchers, the funding organizations, and the policymakers, all working together to be able to accelerate the progress towards the goal of making cancer screening and treatment accessible for all.”
But don’t wait to think about your future or your health and cancer prevention. Start today with small steps.
“One of the things that people can do now is address these preventable factors. We know, for example, that a lot of cancers are related to tobacco smoking. We know that if you are obese or overweight, or have diabetes, these are risk factors for cancer. And this disproportionately impacts the Hispanic and Latinx community.”
Take measures to manage these preventable risk factors. Maintain a healthy diet. Stay active. Stop smoking. See your doctor. Pay attention to changes in your body. And that includes seemingly unrelated infections.
“There are also cancer-causing infections, and if you have these infections, you might be at an increased risk of cancer later on. You can get vaccinated to prevent some of these infections, and if you do have an infection, make sure you get it treated so that you don’t have an infection that continues in your body. Addressing these preventable risk factors is something that an individual can take into their own hands, and it might not seem like it can make a big difference. Still, many cancers can be attributed to these preventable risk factors,” said Dr. Treviño.
Another thing to consider is that medical research needs the Latino community to get involved in preventative care and participate in research when available.
“Minority patients are often not included in clinical trials and medical research, so historically the information from these trials has come from white individuals,” Dr. Treviño added. So, there’s still a lot that experts don’t know about minority risk factors and unknown risk factors that they are still learning about.
From a survivor’s perspective, knowledge is power, and taking your health into your own hands is essential. As a colon cancer survivor who never thought she was at risk and had no symptoms of the disease, Yla Flores is living proof of the necessity of screenings.
“Speak to your doctor, and don’t miss your screening timelines. If you have symptoms, ask questions – you may need to advocate for your own health. The truth is you never think it’s going to happen to you, but then it does. People are getting diagnosed younger and younger. This is no longer an ‘old person’s disease. We need to fight and figure out what is happening in our society that is causing colon cancer to rise.”
Disclaimer:
This story reflects one individual’s experience. Not every person will have the same treatment, experience, outcome, or result. Cologuard is prescribed by your health care provider. Talk to your health care provider about available screening options and whether Cologuard may be right for you. There are potential risks associated with the Cologuard test, and it may not be appropriate for all patients. For more information about the risks, talk to your health care provider or visit Cologuard.com/risk-information for more information.
Cologuard is intended to screen adults 45 years of age and older who are at average risk for colorectal cancer by detecting certain DNA markers and blood in the stool. Do not use if you have had adenomas, have inflammatory bowel disease and certain hereditary syndromes, or have a personal or family history of colorectal cancer. Cologuard is not a replacement for colonoscopy in high-risk patients. Cologuard performance in adults ages 45-49 is estimated based on a large clinical study of patients 50 and older. Cologuard’s performance in repeat testing has not been evaluated.
The Cologuard test result should be interpreted with caution. A positive test result does not confirm the presence of cancer. Patients with a positive test result should be referred for diagnostic colonoscopy. A negative test result does not confirm the absence of cancer. Patients with a negative test result should discuss with their doctor when they need to be tested again. False positives and false-negative results can occur. In a clinical study, 13% of people without cancer received a positive result (false positive), and 8% of people with cancer received a negative result (false negative). Rx only.
For Image credit or remove please email for immediate removal - info@belatina.com