6Research, past and present, has demonstrated psychedelics
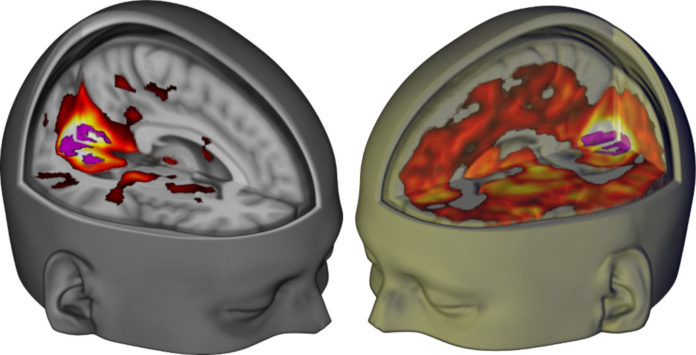
Research, past and present, has demonstrated psychedelics’ unique capacity to treat mental health conditions. However, psychedelics are considered a Schedule I drug by the Drug Enforcement Agency, meaning that the federal government believes that psychedelic compounds have a high risk of abuse, are unsafe to use even under close medical supervision, and have zero medical use anyway.
If you’ve ever done psychedelics (between 10 and 15 percent of the U.S. population aged 12 and older have used a hallucinogen at some point in their lives), you’re likely aware that the government has given these compounds an undeservedly bad rap. After all, psychedelics were largely banned to maintain social order, according to the Multidisciplinary Association for Psychedelic Studies, or M.A.P.S.; in the 1960s, when hallucinogens became widely used as a recreational drug, critics seriously warned against the breakdown of society: “We have seen something which in a way is most alarming, more alarming than death in a way. And that is the loss of all cultural values … these people … are deculturated, lost to society, lost to themselves.” It wasn’t until recently that psychedelic plants and drugs started making a resurgence in the contemporary medical community among the general public, despite the stigma that psychedelics are somehow bad, dangerous, or only for tuning way out.
Much of this can be attributed to the sustained effort by M.A.P.S, a non-profit research organization, to continue to carry out well-designed studies that reaffirm the medical potential of psychedelic plants and drugs. The prevalence of addiction, anxiety, depression, and PTSD is on the rise in our era, with rates rising faster than traditional medicine has been able to adequately treat these illnesses; tired of suffering from these conditions, people are desperate for effective, safe, and accessible alternatives to conventional treatments. Even the most unassuming patients are now warming up to using psychedelics as medicine.
From synthetic compounds like LSD and MDMA to plants that can be found deep in the jungle or even in your backyard, here’s a rundown of how psychedelics can be used to treat some of the most pressing mental conditions of the era.
5Treating Alcoholism with LSD

Lysergic acid diethylamide, otherwise known as LSD, otherwise known as acid, might have you thinking more about crowds of hippies tripping their brains out at Woodstock than psychedelic medicine. But LSD is the OG clinical drug of the psychedelic world, the granddaddy of all modern psychedelic research, with purely medicinal origins. It was demonized in the late 60s when Timothy Leary — a trained psychologist, self-fashioned psychedelic researcher, and one of LSD’s original proponents — began to bait the media with far-out statements about the drug; by 1970 the federal government classified psychedelics as illegal, dangerous drugs.
It’s a crying shame because, prior to its ban, LSD has helped researchers discover how depression works, and even more importantly, revealed for the first time that mental illness could be modulated through changes in brain chemistry, one of the major neuroscientific breakthroughs of the mid-20th century.
Classic studies utilized LSD to treat alcoholism. Contemporary researchers have run analyses on these historical studies to confirm that LSD is an effective treatment to the illness, finding that nearly 60 percent of alcohol abusers were able to cut back on their consumption after taking a single dose of LSD. The positive effects on participants’ relationships with alcohol lasted for some time — about six months — but dissipated within a year of dosing, suggesting periodic treatments are the way to go.
Disclaimer: ever heard of acid flashbacks? It’s a thing to relive the experience of your acid trip, months after you took it. And while most people can take LSD safely, it can trigger psychotic breakdowns in certain users, so you’ll want to find a psychedelic specialist who is well-studied in the drug’s contraindications before using LSD in moderate-to-large medicinal doses. Microdosing, on the other hand, won’t have you tripping in the least; researchers are just beginning to delve into the cognitive benefits of low doses.
4Treatment-Resistant, Severe Depression

Ayahuasca, an entheogenic brew of plants from the Amazon, has historically been used as spiritual and medicinal healing by its communities. Typically, an experienced shaman leads the user through a psychedelic journey that plumbs the depths of both the soul and the universe. The introduction of this inimitable experience to a global audience has made it so popular that it faces extinction in the wild. As herbalist Sarah Wu emphasized to us in a recent interview, “[Leave] certain medicines for the sick.”
As medicine for the modern patient, ayahuasca has demonstrated the almost miraculous capacity to treat severe depression. Most recently, a small Brazilian study published in Psychological Medicine concluded that ayahuasca effectively relieved the symptoms of patients who suffered from treatment-resistant depression. Under calm, journey-inducing settings and close observation, over half the study’s participants were able to see significant improvements in their condition after just a single dose, even a week after receiving treatment. (The study did not observe patients beyond day seven.) The researchers’ findings supported a previous study in which ayahuasca acted as an antidepressant, lifting the weight of depression of its users within the first hour of dosage and lasting for three weeks following the treatment.
Even ketamine, known recreationally as Special K and originally formulated as a tranquilizer for animals, has its uses in the treatment of depression. Recent studies have found that within hours of receiving an infusion of ketamine, patients whose illnesses resisted traditional treatments no longer experienced symptoms of depression. The effects were neither permanent nor without side effects, but the preliminary research surrounding ketamine has experts inching closer to addressing the root causes of depression. In another study, ketamine also acted quickly to treat severe, treatment-resistant depressed bipolar disorder, working within an hour of the infusion of the drug and lasting for up to two weeks.
Disclaimer: It’s well worth noting that ayahuasca should not be taken casually. It can negatively interact with certain foods and drugs that contain monoamine oxidase inhibitors — including some kinds of antidepressants — and should definitely not be taken by patients with a history of psychosis. People have been permanently messed up and have even ended up dead after taking ayahuasca, so don’t look to this as medicine unless you’re with a skilled healer who is able to assess these known risks.
3Mortality-related Depression and Anxiety

One of the safest, most accessible psychedelic medicines can be found flourishing in cow patties. Hallucinogenic mushrooms. A 2017 report concluded that mushrooms are the safest recreational drug of all, even safer than marijuana (which hasn’t killed a single person in the history of its use).
Most people who take mushrooms are introduced to these bitter-tasting fungi for a fun night full of trippy hallucinations and visions triggered by the environment around them, but recent research has uncovered the medical potential of this humble shroom. Psilocybe, a class of psychedelic “magic” mushrooms, contains a compound called psilocybin that has been the subject of promising studies to treat anxiety and depression (stemming from diagnoses of terminal illness).
One study from 2016 focused on people who were suffering from anxiety and depression due to diagnoses of terminal cancer. Following a single large dose of psilocybin, a majority of the study participants experienced significant relief from the symptoms of depression and anxiety that had previously affected their quality of life, and not just while they had the compound in their system; over three-quarters of the participants saw improvements in their symptoms long after their treatment, experiencing positive effects up to half a year later. Notably, about 70 percent of the participants, while faced with their assured mortality, reported that their experience with mushrooms was one of the most meaningful and spiritually significant experiences that they’d ever had in their lifetimes.
2Smoking Addiction

Preliminary research has indicated that mushrooms may be by far the most effective drug available to help people quit smoking. A small study from 2014 found that after a few scheduled doses of psilocybin, 80 percent of its participants — smokers who had previously been unable to kick the habit — still hadn’t smoked a cigarette at the six-month follow-up. Compare that to a 35 percent success rate with varenicline, the drug currently prescribed to smokers trying to quit.
It’s not that the mushrooms themselves were inhibiting cigarette addiction, but rather facilitating the cessation of smoking. The study’s participants were periodically using the drug in tandem with weekly, one-on-one sessions of cognitive behavioral therapy. “When administered after careful preparation and in a therapeutic context, psilocybin can lead to deep reflection about one’s life and spark motivation to change,” explained a co-author in a press release following the conclusion of the study.
1Post-Traumatic Stress Disorder
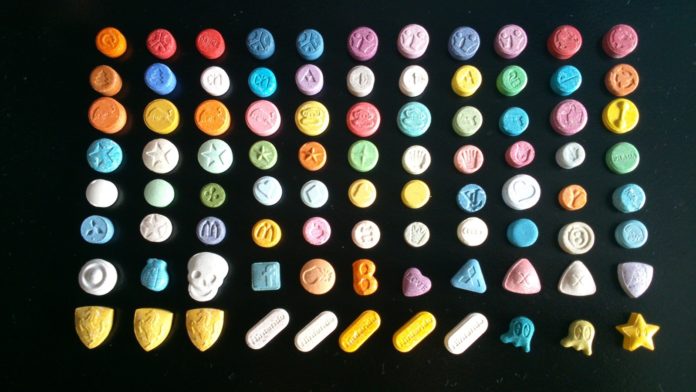
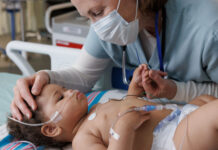
MDMA, otherwise known as ecstasy or molly, can be way more than just a party drug, according to results from preliminary studies. Used as a psychedelic medicine, MDMA can be a godsend for people suffering from PTSD, in some cases “curing” them altogether of their symptoms.
A study published last year treated fire fighters, police officers, and military veterans who were suffering from chronic PTSD. None of the participants had been able to find relief through traditional methods of treatment. Following several treatments with MDMA though, a majority of the participants found significant relief of their symptoms, as well as improvements in sleep quality, with only one person experiencing an adverse event that possibly was related to the drug. (Any other negative effects were minor, dissipating within days following being dosed.) At the one-year follow-up, participants’ PTSD symptoms had been reduced to the point that over two-thirds of them no longer fit the criteria for having PTSD. The results from this study were so promising that the Department of Veterans Affairs has begun designing their very own studies of the drug.
As with mushrooms, MDMA was administered to patients in an environment conducive to a good trip — candles, flowers, music — in tandem with guided supervision during the trips a well as ongoing psychotherapy. At therapy sessions, the patients explore their trauma with a sense of trust and well-being that was unlocked by the drug. “The MDMA seems to act as a catalyst that allows the healing to happen,” explained one of the study’s lead researchers in an interview with the New York Times.
Final Words
In his new book “How to Change Your Mind,” Michael Pollan quotes a researcher who describes psychedelic drugs as ”placebos on rocket boosters.” In other words, it’s not the psychedelic drug that is “fixing” the patient but rather its combined benefit with psychotherapy that is effectively managing or treating the patient’s condition. I cannot stress that point enough.
That means you shouldn’t reach out to your tripper friend for his or stash of recreational hallucinogens; they aren’t the “miracle pill” that you’re looking for, merely a means to an end. More importantly, in the wrong environment and without a good “guide,” you may end up exacerbating your health condition, and sometimes permanently. Instead of venturing into psychedelic treatments on your own, you will want to seek out a professional therapist who has experience with hallucinogens. Administered with care and regular therapy sessions, psychedelics could having you tripping your way to better mental health.
Disclaimer: Psychedelics are illegal. This publication is does not advocate the use of any illegal substances.
For Image credit or remove please email for immediate removal - info@belatina.com