May is Mental Health Awareness Month. I was unaware of this until this morning, when I began to write up a brief rundown of barriers that prevent people from receiving treatment for their mental health conditions. Stigma, structural barriers (like proximity to treatment or simply having enough time in the day to get to an appointment), cost, and mental health illiteracy are four prominent reasons why people are not getting treatment for their mental health conditions, whether from a psychiatrist, therapist, or at an in-patient center.
One way to counteract stigma surrounding mental health is to share your personal mental health experiences with others, so here’s some of my story.
The Serious Setback of Mental Health Illiteracy
As the daughter of a Korean immigrant, I have encountered my fair share of stigma over my experiences with anxiety and depression. I suffer from anxiety that can, under the right circumstances, boil over into panic attacks or days-long stretches of depression. When I first opened up about my struggles with my mother, she brushed it off as self-pity, or simply my being too sensitive to normal, societal pressures. After all, everyone has to contend with the pressure to be successful or happy or perfect. In her mind, my distress was unremarkable, not a sign of mental health issues.
Like any good Korean child, I grew up playing classical piano. In middle and high school, I had a very demanding piano instructor who never spoke of piano as a fun pastime. Instead, she endeavored to sign me up for competitions. I attended a few of them and scored well, but I began to dread the day before or even the day of my performance. I would force my mom to call and cancel, and then I would lie in bed and wait for my time slot to pass before being able to clear my mind. Neither my mother nor I were able to identify this pattern of behavior as an indication that I was panicking. How could we? Neither of us knew what anxiety was. We were illiterate in mental health.

Consider how you might be able to recognize that you experience feelings of despair. Will you be able to discern whether you are just having a bad week or are suffering from depression? Perhaps you feel yourself having unexplainable mood swings. Will you identify that as a potential sign that you suffer from bipolar disorder, or will you just believe yourself to be uncontrollably irrational? Do you suffer from OCD? Or are you just a run-of-the-mill germaphobe? There are a myriad of scenarios that illustrate how not having a basic understanding of mental health puts people at a disadvantage right from the get-go. After all, if you don’t know that you are suffering from a mental health condition, how can you even begin to treat it?
The Breakthrough of a Breakdown
A decade elapsed before I could put a name to my experiences as an amateur pianist. It took me having my first panic attack in New York City to understand that I had been experiencing something that was “not normal” at different points in my life. I used to work in a popular restaurant where I would show up to work, inheriting a 2-hour waitlist from the day manager, along with all the icy glares from people who were impatiently waiting for me to call their name. One evening, I distinctly remember being unable to leave the office to get onto the floor of the restaurant. It was more than just a feeling of “I don’t want to deal with this today.” It was, rather, a paralyzing fear that left me in tears. I began hyperventilating. I felt glued to the chair, and I remember wondering, “Why can’t I move?”
Fortunately, a coworker of mine came into the office and saw what was happening. “You’re having a panic attack,” he said matter-of-factly. “My wife gets those.” He brought me a small glass of beer, told me to drink it and take ten minutes to calm down, and then made sure I was okay before letting me start my shift. I know now that my panic attack was the culmination of my inherent anxiety issues, plus stress, lack of sleep, having no time to relax, and the feeling that one false move would cause everything around me to crumble into a cataclysmic failure.
I had no reason to know that what I was experiencing panic attack symptoms then and as an adolescent, and I might never have known that I was having a panic attack if my coworker hadn’t had found me in the middle of one. I had taken psych classes in school and was aware that the brain works in mysterious ways, but personal mental health was never discussed at any point in my education.
The Stronghold of Stigma
I shared these revelations with my mother, but it took several phone calls with her to get her to actually hear me. I would have seriously been hurt had I not prepared myself for her response; I knew that I could expect love, but not necessarily acceptance or comprehension. The reality is that not everyone is literate in mental health, including your closest loved ones, and they may fall back on stigmas in order to make sense of your condition. Frankly, this possibility is terrifying and can seriously discourage people from getting help. What if people start treating you differently? What if they attach hurtful adjectives to you? What if they think less of you?
In my case, once my mother accepted that I did indeed have issues, she began to make my mental illness about herself, wondering what she had done wrong. As if mental illness is necessarily the result of someone being at fault. She went down the list: Was I the victim of abuse? Of neglect? Of trauma? No, no, and no. Then she began to wonder aloud if my job, my husband, or my friends were behind my mental illness. No, no, and no, I would insist.
My mother would get frustrated and say to me, “Do you understand the pressure that kids face in Korea? You’re lucky you grew up the American way.” She lives under the impression that every kid in Korea turns out just fine, despite being subjected to an infinitely more demanding upbringing than I had. The statistics, however, illustrate a completely different picture than the one she has in her mind, demonstrating how easily our conceptions can be so far removed from reality. According to figures cited by a 2017 article in Berkeley Political Review, South Korean children between the ages of 10 and 19 face the highest suicide rate in the world; a majority of these suicides are the result of stress from the pressure to succeed in school, the very same pressure that my mom had referenced in trying to explain my anxiety away. Knowing how my mind works now, I realize that I am, in fact, incredibly lucky to have grown up “the American way.” I very well could have been part of that suicide statistic.
Generally speaking, this perception that everything is “just fine” is partly the result of a closed dialogue around mental health. No one in Korea airs their “dirty laundry” for fear of being shunned or judged. There’s also a pervasive sense of shame and weakness over not “being able to handle” circumstances that your peers take in stride — even if they really aren’t. Distress is explained away as physical ailments or normal emotions rather than symptoms of an underlying mental condition. These stigmas and misunderstandings are prevalent in the Latino community, too.
In Korea, the dialogue around mental health has begun to change as celebrities and K-pop stars open up about their mental health issues, and that has genuinely had influence over my mother’s acceptance of my experiences with anxiety. I know that celebrity testimonials sound like they should be pretty inconsequential in the grand scheme of things, but having high-profile, open dialogue about the subject is a major balm to stigma, especially when we hear it from people we value and respect. We’re starting to see it more and more among prominent Latinos who are in a position of influence. Bad Bunny frequently references his depression in his lyrics. J Balvin, who just earned the award for Best Rap Song at the Billboard music awards, has for years been open about his anxiety. He told Fader in 2016 that he sometimes has panic attacks, bouts of dread, when he’s working too much and not getting enough sleep. “For two months afterward [my first panic attack,] I was in hell. I lost the desire to live,” he shared. “I went to lots of doctors and tried alternative medicine. I didn’t want to go to a psychiatrist because I thought it was for crazy people. And it turned out I was crazy.”
The Importance of Discussing Mental Health At Home
Mental health was never discussed in my family, even though it was clearly a relevant issue. Both my father and his father struggled with addiction. My grandfather, for one, was an alcoholic. My father, knowing that his father abused alcohol, was able to recognize when his own relationship with alcohol was becoming toxic and never touched liquor or booze. Instead being an alcoholic though, my father was a heavy smoker who tried and failed to quit many times throughout his life, ultimately losing his life to lung cancer. I find myself explaining to people that addiction is what destroyed him, not cancer.
Neither of my parents gave my brother or me the courtesy of sharing our family’s mental health history with us, perhaps because they didn’t know that it could be relevant to our mental well-being. Or perhaps stigma prevented them from sharing my father’s conditions with us, fearing that we would think less of him. Our upbringing was comfortable and loving, so why even bring up the bad stuff? Why put those thoughts in our mind? There was “no reason” why either my brother or me or even my father would need to be experiencing mental anguish.
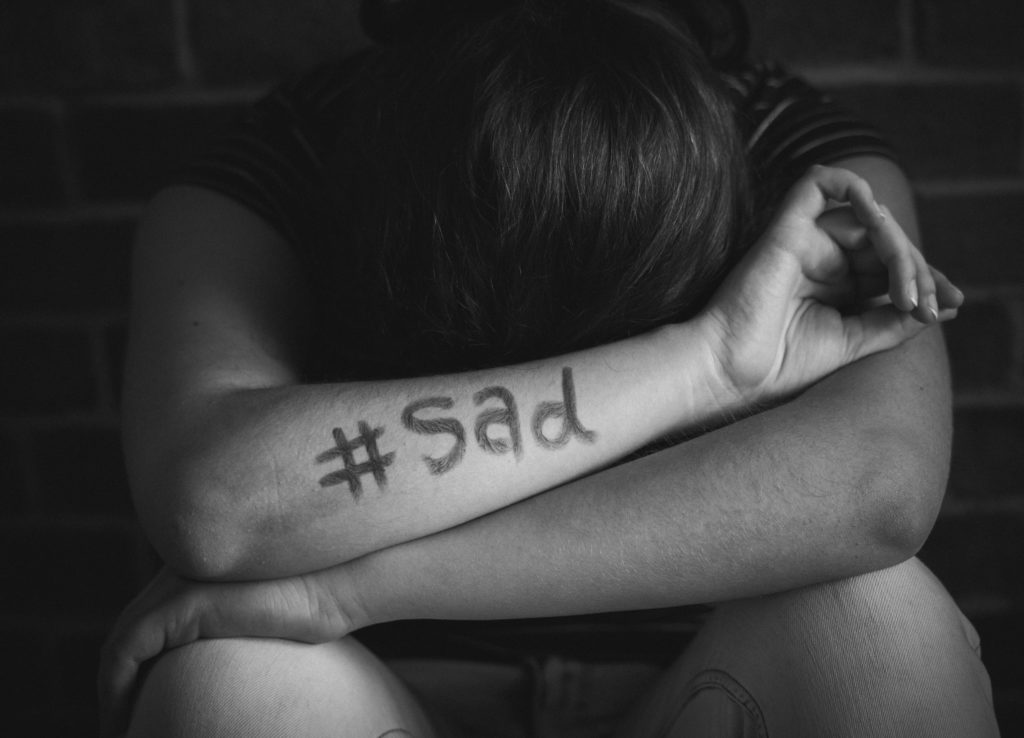
Except mental health doesn’t work that way. Mental health doesn’t need a reason to exist when there are hereditary factors at play. It wasn’t until maybe three years ago that my brother and I discovered that we both struggle with anxiety and depression. I remember exclaiming to him something along the lines of, “You experience suicidal ideation too?!” like it was a relief. I had connected with friends over that revelation before, but knowing that my brother was susceptible to the same pattern of thought made me feel like I wasn’t crazy. Or rather, that I was crazy, but that I didn’t have to shoulder that irrational, potentially life-threatening inheritance alone.
The two of us don’t know for sure, but we both suspect that we inherited these conditions from our father who, to reiterate, was never diagnosed for depression or anxiety and rarely spoke of his own feelings. It wasn’t even until the last week of his life that he revealed to me that he had been abusing alcohol early on in his marriage to my mother, that his disordered drinking was a result of him feeling isolated while living as a foreigner in Seoul, Korea, a captain in the military. I was eight at the time and would never have known about this had he not opened up to me about it. When I asked my mom about this period of alcohol abuse (they had been divorced for many years) she outright dismissed that my dad had ever had a problem. Maybe she really didn’t know. Or maybe old stigmas die hard.
Implementing Mental Health Literacy Into Society
At this point, I have literally learned everything I know about mental health from the Internet — there are so many amazing resources out there — or from friends sharing their own experiences with me. There’s great value in being self-sufficient and having a healthy forum to talk casually about mental illness, but it’s clear that we ought to be receiving a formal education in mental health. Public health officials are beginning to convince schools to integrate mental health curricula into their programming as a way to expand this mental health literacy. Last summer, New York and Virginia became the first two states to mandate mental health education into public schools in response to the prevalence of suicide in adolescence. CNN cited CDC data that named suicide the second leading cause of death for people between the age of 15 and 24, while Latino youth are more likely than their peers to attempt suicide.

An organization called Mental Health First Aid offers training to members of the public who want to have basic skills in identifying and understanding mental illness among members of their community. Walgreens recently partnered up with the organization to expand the opportunity for their pharmacists to receive mental health first aid training as a way to better serve their patients who may be dealing with mental illness or addiction. It’s not just for health professionals: as an individual who doesn’t work in the health industry, you can search their database for places where you can complete a free, 8-hour training course in mental health first aid. Think of it as CPR training, but for mental health.
Cost and Structural Barriers to Mental Health Treatment
After years of not being able to afford decent health insurance, this year was the first year I was able to fit a “silver-level” plan into my budget. As such, I finally decided to see a primary care physician, relieved of the fear that I would somehow be expected to pay for something that I couldn’t afford. I had never met my PCP before, so I had to run through my family’s health history. My heart pounded as I gathered up the courage to tell her that I suffered from anxiety and depression, that it likely ran in my family. Telling a complete stranger who had not yet won my trust was nerve-wracking. Was she looking at me as a human, or as one of the freaks that she had read about in her training? I was surprised to be falling back on stigmas that I thought I had overcome.
But, like a good doctor should, my PCP typed brief notes into the computer and nonchalantly asked me if I wanted a referral to see a therapist. I said yes. She warned me that finding a therapist that was covered by my insurance policy would be difficult, and that I was probably better off paying out of pocket if I could find someone to recommend a good provider. Beyond that, finding a therapist would be very much like dating. “It’s rough out there,” she said.
My PCP’s point was that just because someone has been trained to understand a clinical diagnosis doesn’t mean that they’ll be a good fit for you. This is true in general. But this is also a unique barrier for Black and Latino patients, since mental health care is just as susceptible to racial biases as physical health care, leading to inadequate treatment. “[Systemic racism] means there’s a lack of access to proper mental health care, cultural biases from health providers, misdiagnoses such as attributing certain behaviors to delinquency as opposed to survival coping strategies for the trauma people have faced,” explained Shardé Smith, a University of Illinois professor of human development and family studies, in a recent interview with Illinois Public Radio. Systemic racism in health care is not an issue for me, but I have a feeling that a mental health professional that has experience working with immigrants will be better able to guide me to tools that I’ll need to cope with the cultural dissonance I experience when discussing my mental health with my mother. As with any field of work, representation matters.
Feeling like I was making progress with my mental health, I made a few calls to my PCP’s referrals but was promptly discouraged: all of the names that she had given me did not take my insurance. This, apparently, is typical. In 2017, the National Alliance for Mental Illness published a survey that found that over a third of Americans who seek mental health treatment encounter this barrier to treatment. When patients seeking mental health care were rebuffed, it was most often due to the fact that the psychiatrist they were hoping to see did not take their health insurance. Of survey respondents who did manage to arrange psychotherapy, almost 30 percent ultimately ended up using an out-of-network provider. In contrast, the vast majority of Americans have no issue finding a PCP or specialist who will take their insurance, illustrating a significant disparity in care for mental versus physical health. That conundrum can reinforce the stigma that physical ailments are cause for real concern while mental ailments are not.
Medicaid recipients have better luck finding in-patient mental health care and are less likely to have to pay out of pocket, but they still face barriers to receiving treatment. About a quarter of Medicaid recipients reported that potential out-of-pocket costs for mental health care deterred them from seeking treatment, suggesting that implementation of out-of-pocket costs could have a significant influence on the mental well being of low-income communities.
As if insurance coverage isn’t a big enough challenge, one of the most common barriers to finding a psychiatrist or therapist is the fact that many are not accepting new patients. This is due in part to the fact that there are more patients than providers. The NAMI report cited a mental health workforce shortage that has severely limited who gets to be treated for their mental health conditions. An estimated 91 million people live in communities that lack adequate access to mental health care. Over a third of survey respondents simply do not live or work close enough to a provider to fit mental health care into their lives.
I live in New York City, a high-density metropolis where I can walk to just about any basic amenity that I need access to, and yet commuting to and from any of the therapist referrals that my PCP had given me could very well cost me at least an hour of my day, not including the appointment itself. I don’t have dependents, so I don’t need to worry about arranging for childcare. I also mostly work from home and have a flexible schedule, so I don’t have to ask for time off of work. And yet, I have started to feel like seeking mental health treatment is just too much of a hassle. “I don’t really need it,” I find myself concluding. While that might be true most of the time, what about the times when I’m experiencing a mental health crisis? I’m doing myself a huge disservice if I don’t set myself up for success when shit hits the fan. Because, in this life, it will.
All told, it’s clear that mental health care needs to undergo a major evolution if we expect it to serve an American public that is in dire need of treatment. Telemedicine, perhaps, could be a novel solution to the challenge of expanding access, reducing costs, and tailoring treatment to mental health patients’ needs. A review published in 2017 concluded that telemedicine—meaning, sessions conducted over the phone, over a live chat, or through a video conference — is just as effective as in-person sessions, and has the added benefit of reaching patients who live in mental health care deserts. Moreover, telemedicine opens up the possibility of offering futuristic-sounding things like analyses of your facial expressions as a way to reinforce diagnoses or help monitor your course of treatment.

In the meantime, when I start to feel overwhelmed, I clutch my clear quartz to my heart like it is an Infinity Stone, make a pot of tea, and diffuse some lavender oil. It’s no substitute for a solid therapy session, but I’m grateful to more or less be able to cope with mental health issues on my own. Which is pretty much what the understaffed, underfunded, underequipped mental health industry in America is hoping I can do.
For Image credit or remove please email for immediate removal - info@belatina.com